What is a Rhinoplasty and what does it involve?
Of course, this feeling is generated by the media which have unintentionally stigmatised rhinoplasty by associating it with celebrities who are already objectively good looking who have a rhinoplasty as a cosmetic procedure to serve their vanity. However, in the cleft and craniofacial world, a rhinoplasty has its place as an important procedure for both cosmetic and functional reasons. A rhinoplasty is generally done as one of the final procedures once you’ve finished growing.

In my case, a rhinoplasty was a procedure that I had wanted for a long time. It was a procedure that would build on the previous orthognathic surgery that I had had and make my face that bit more symmetrical. Like with any procedures, when I was considering whether to have the surgery, I asked myself what the goals of the procedure would be. For this, there were three. The first was to make my nose more symmetrical and to have a shape that was a bit more typical. The second was to make my nose smaller – I had been teased for many years about the size of my nose and I had become self-conscious of my nose and I was worried that people were fixating on it when I was meeting them for the first time. This was impacting on my confidence in new situations, and I felt that I had to over compensate for looking different. The third goal of a rhinoplasty was a very functional goal of improving my breathing. My right nostril was collapsed which meant that I could not breathe out of it. By opening it out, it should improve my breathing as I could breathe through both nostrils and less through my mouth which had been resulting in a dry mouth and a poorer air quality (when breathing through your nose, it acts as an air filter, catching a lot of pollutants before they enter your lungs).
In addition to doing the rhinoplasty, the team thought that it would make sense to make a fifth attempt at repairing the fistula that was in my palate.
The Day of Surgery – Thursday 1 December 2016
It was officially the first day of the New Zealand summer as I headed into the DOSA (Day of Surgery Admission) unit at 7am in Christchurch Hospital. Like I’d done a couple of times before, I got changed into my gown and stockings and curled up in the bed waiting for the various team members to come and see me. The anaesthetist came to see me, and I explained to him about my needle phobia and that I would prefer a gas induction. I also negotiated with him to not use a catheter if it could be avoided. Next, the registrar and my two surgeons came around to re-explain what they were doing with my nose – a procedure called an open rhinoplasty. I won’t scare you with the gory details, just remember that it is pretty routine and that you’re asleep when they do it! They also made a somewhat rash decision to attempt a repair on my palate at the same time. This was a little odd as they hadn’t done any preparation work for this, but they appeared fairly confident with what they were doing, and so I consented to this.
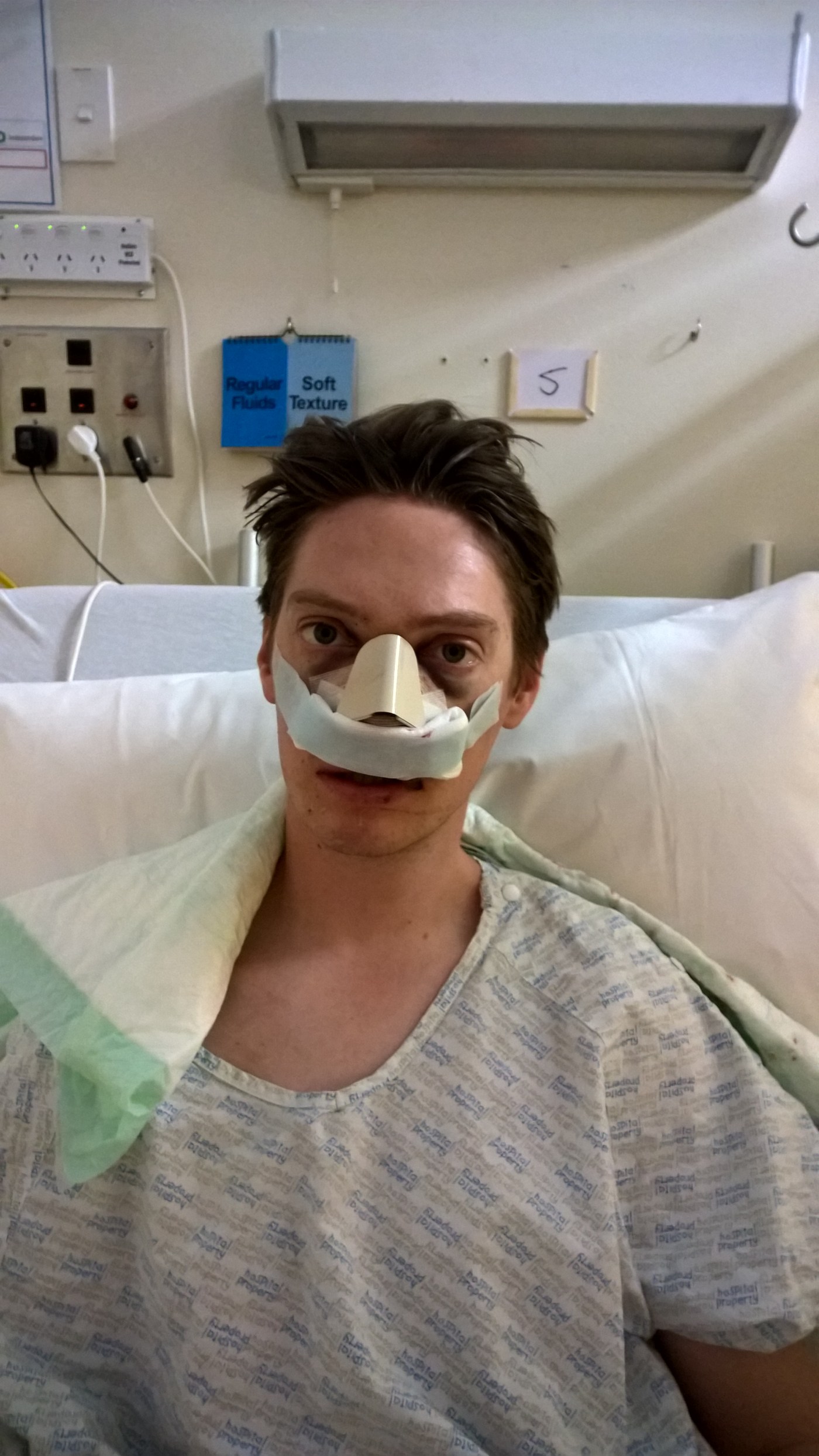
I was wheeled down to theatre a few minutes before 8am, and felt at ease as I started inhaling the gas, knowing that I’d been here many times before and was in safe hands. When I woke in the recovery ward, it was about 12.35pm and I was surprised to find an oxygen mask on my face – I was used to this from previous procedures, but was surprised to find one over my nose when they’d just operated on my nose! A recovery nurse called Dawn was there when I came around and could sense that I was a naturally anxious person and knew all the right things to say to calm me down. I remember others being a little concerned about my high heart rate and she said to me “Don’t worry. It’s just like you’ve run a marathon, but it’s fine, because when you go to sleep, it drops back down.”
After a little while there, a nurse called Jess came down to wheel me back up to recovery and she kept an eye on me for the rest of her shift. My team at work had generously put together a care package for me which included one of my favourite magazines, National Geographic. It had a feature on how we could build a colony on Mars. Jess, who would also have been in her twenties was also a huge fan of space and she sat down to go through the magazine with me when she had a little bit of downtime. It may seem like a small thing, but those little efforts of taking the time and showing compassion make all the difference.
Recovery

I was quietly optimistic that I would get to go home the next day, as I didn’t really fancy being in hospital over the weekend, but when my surgeon came to visit the next day, he explained that it would be wise to stay in another night. He explained that the surgery had gone well but was far more complicated than they were anticipating due to a large amount of scar tissue left over from a previous surgery I’d had on my nose at age 10. They removed a 5cm piece of bone from my nose and had seriously de-bulked my nose. He explained that unfortunately they hadn’t been able to open my right nostril as it was so severely blocked, which can’t be helped. This was certainly a disappointment as all the promises of clear airways, more effective breathing and an end to the dry mouth had now been dashed, but I have learned to become more philosophical about it and accept that if anything could have been done, it would have been done, and that at least I have one functioning nostril!
Like anyone would be, I was eager to see the results of the surgery for myself and take a peek at what my new nose looked like; be warned, patience is required here! My nose was underneath a nose splint, this stays in place for two weeks to ensure the nose sets in the desired position. So until then, all I could see in a mirror was a massive splint staring back at me, and I had bruising under my eyes – I looked a lot like a raccoon.
Also, imagine your worst cold when you are all bunged up and despite your best efforts can’t clear your nose. This is what it is going to feel like for a little while as special dissolvable nasal tampons are placed up your nose to absorb blood and reduce any post-operative bleeding (and as a guy, having a personal anecdote to contribute to a conversation about tampons is invaluable). Unlike Tampax, these special nasal tampons are coated with a cocaine-based analgesic to help with the pain. So you also get an anecdote about snorting cocaine. For those who don’t already know me, I’m about as risk-averse as they come with regards to drugs – my own medical experiences have been enough to put me off taking any unnecessary drugs (well, except for a casual drink, I do enjoy one of those), so you can imagine the genuine intrigue in the room when I tell people about the time that I snorted cocaine off a tampon.
Although the tampons are dissolvable, in my case, once they’d served their purpose, they did need a little bit of encouragement to come back out again. I was really anxious about what this may involve, but it really was painless and nothing to worry about. In fact, when the nurse pulled them out (layer by layer), there was an overwhelming sense of relief as I could breathe more easily again (even if it was just through one nostril).
Another post-surgical anxiety of mine was stitches. The surgical team had used a combination of dissolvable stitches (for the palate repair) and non-dissolvable stitches (for my nose). I soon realised that there is a large variation on the amount of time for a dissolvable stitch to come out – some of them came out as soon as 10 days after the surgery, while some neighbouring ones took more than six weeks. As for the non-dissolvable ones, they removed some of these at 7 days after the operation. This was proving to be quite painful which indicated to the nurses that they weren’t quite ready to come out. They got me back a week later and took them out with minimal pain. Be sure to communicate if you’re in pain when stitches are being removed.
After two nights in the hospital I was sent home late on Saturday the 3rd of December. As I lived alone at the time, I went back to my Mum’s house in the initial stages of my recovery (my Mum is an incredible person who has undoubtedly gone through a lot over the years to tend to my healthcare, and even at this age would happily look after me while I was convalescing)! As incredibly grateful as I am to my Mum for looking after me, I was used to being independent (and Mum was used to having her space) and so I was keen to get back to my own place as soon as I was fit enough. This was assisted by nurses who would do home visits to change my dressings and observe my wounds. This was a really hit and miss endeavour as some nurses were great while others clearly had no experience with cleft (I had been prescribed ointment for the stitch (suture) lines on my nose, and one nurse was convinced he needed to put the ointment in my eyes).

Nine days after my op, I returned home (safe in the knowledge Mum lived just around the corner), and it wasn’t to be long before I picked up that phone. I had been doing my best to sleep on my back so my nose wouldn’t make contact with any bedding or anything else that may cause it harm, yet somehow I had managed to roll onto my side. At about 6.30am on Monday 12th December, I woke up to see my nose splint fall off. I had been under strict instructions not to remove it, so I became quite stressed. I put it back in position and lay on my back until 8am when I could phone the hospital, afraid to move, even more afraid to look in the mirror. The hospital asked me to come in as soon as I could. Upon arrival, the resident took the splint off again, looked at my nose and said “It’s done its job. We can take it away now.” Well, you can imagine my overwhelming sense of relief! She then asked “Are you ready to see your new nose?” – I certainly was keen to see it. She got one of the nurses to clean everything up and get rid of any dried blood etc. and handed me a mirror.

Take a deep breath in. I was amazed at what I saw staring back at me. My nose was obviously swollen, but for the first time ever, it was symmetrical – it looked quite big, but ordinary. I was stoked. This was something that I had been harassed about for as long as I could remember, and now I could see that with time, my nose was going to look like everybody else’s. The surgeon told me that 80% of the swelling will go down after about three months, with the remaining 20% taking about another year, so it’s certainly worth bearing that in mind when seeing your nose for the first time, but you certainly should be able to see enough to picture what it’s going to look like when all the swelling subsides. Of course, it wasn’t perfect – it never will look completely like it would have had I not had a cleft, but it was close enough to make me feel more positive about my appearance and to feel that in terms of surgical work on my nose, we had come as far as we needed to go.
Complications
Of course, like with any surgery, there are always risks. I think when you have lots of operations, chances are at some point you may experience a complication or two. Unfortunately, this rhinoplasty did come with a few.
Gastrointestinal
This was the most severe of the complications, and ironically was the one that had nothing to do with my cleft. It’s worth remembering that just because you have a cleft, you don’t become immune to everything else (unfortunately). On the day that I went home from hospital, I was feeling pretty miserable, but that’s to be expected – I’d had a surgery and very little sleep, I was hardly going to be bouncing off the ceiling shouting Yippee Ki Yay, so I didn’t think much of it. The next morning, I felt very clammy and had my first bowel movement since the operation. It was very watery and bloody, but the first one after an anaesthetic often is very diarrhoea-esque so I thought nothing of it. As the morning wore on, my tummy grew more and more painful and the pain from my stomach was quickly outweighing that of the surgical sites and not nearly being met by the concoction of painkillers that I was on at the time. I went to the toilet about 90 minutes later, and again a watery and bloody motion followed. Obviously, when one is healthy the colon is used to forming solid stools, not firing out liquid. Mum’s bathroom kept becoming a bloody mess every 60-90 minutes and I was getting weaker and weaker. As my nose was all sealed up, I couldn’t smell anything at the time, but I am told the stench of what is known as frank blood is overpowering.
My Mum is the opposite of me when it comes to health related anxiety – she is no hypochondriac. She can reason with you and remind you that a headache is far more likely due to the fact that you haven’t drunk enough water today rather than the brain tumour that you’ve convinced yourself of. So when Mum started to be concerned about this bleeding, I knew things weren’t looking good. She quickly rushed me to Accident & Emergency at Christchurch Hospital (not where you want to be on a Sunday night). Although the initial nurse triaged me quickly and found a room in which for me to lie down on a bed, it seemed to take ages for any nurses or doctors to arrive. Of course, they took so long, I needed the toilet again. The nurse who triaged me quickly gave me a container to collect a sample for testing. Once I came out of the toilet with my sample, another nurse walked by and asked if I was okay (strange question to ask of someone in A&E but in my sickly state I let the irony of her question slide) and I said “I’m a bit worried.” I was waiting for a reassuring comment which I so desperately needed to hear at that time, but instead all she could muster after looking at my container of blood (which was such pure liquid she’d assumed it was a urine sample) was “Yes. I would be too if I was you.”
Eventually the doctor came to see me and took the sample to send away for testing, told me to head home with some paracetamol (the rest of my concoction were not good for my tummy) and to follow up in the morning to see the results of the test. She was far too relaxed, and not in a good reassuring way, but in an “I am way out of my depth here” kind of way.
Mum took me home, and then straight to my own GP at 9am the next morning, and she was fantastic. She examined the test results which had tested positive for Chlostridium Difficile. This is a very nasty infection, that I later found out (once I had recovered) from the doctor kills 30% of people who contract it. It had come about due to me having been given a massive dose of antibiotics during my surgery which had also wiped out all the good bacteria in my stomach. I had then come into contact with the infection in the hospital ward and it had taken hold as I had none of my own bacteria left to fight it off. She prescribed antibiotics to fight the infection, and electrolytes to replenish the nutrients I was losing. Within a couple of days, the explosive diarrhoea began to slow down and within about 5 days I was back to a much more normal digestive function. It was only then that my body could properly go into repair mode and begin focussing on recovery. Although technically nothing to do with the cleft, it was a brush with my own mortality that was a little bit closer than I feel comfortable with.

Rosacea
This complication is a lot less life threatening, but a lot more long term. Rosacea is a rash of the central face that lots of people have and is common following the menopause (maybe my use and subsequent cessation of tampons had tricked my body into thinking it was going through a menopause). It is characterised by redness and often quite prominent blood vessels. For me, it started appearing on my nose and my cheeks. Looking back through photos, it has been there for a few years, but has become more profound following the surgery. Commonly blushing due to social anxiety is one possible cause of rosacea, and I know that I used to do this a lot as an involuntary response when I felt uncomfortable (and of course, thinking about it only made it worse). It has now got to a point where, reluctantly, I now need to manage it with daily medication (which does help to prevent my skin from peeling) and moisturiser. On occasions where I feel appearance and first impressions are quite salient, I do envy the option available to women of using makeups, foundations and concealers to cover the rosacea. It is possible that laser therapy could be used to deal with it in the future, but for the time-being, I am content using less invasive methods.
Pesky Fistula
Sadly, I probably could’ve put money on this one being a problem from the start. This was attempt number five at closing the palate, and sadly, the flap that they created died shortly after the operation leaving a large concavity with a smaller fistula at its apex. Whilst the small fistula hole itself is not too problematic, the deep concavity is a nuisance as it becomes a storage hub for some food items, and also makes it nigh on impossible to get at the back of my top teeth with a toothbrush in any meaningful way. Again, this is something that potentially a surgical intervention could resolve (by way of a very invasive tongue flap). At this current point in time though, I feel another surgery is a bit of a gamble. With regard to the fistula, this fifth attempt has made the problem worse, not better, but I have come to terms with that and make adjustments in my day to day life for that (e.g. eating food carefully to reduce the amount that gets stuck and to prevent injury by a sharp or pointy piece of food). I know that I would find it very hard to cope with a situation that is any worse than the current situation and so for me the potential benefit of it being resolved is not worth the anguish of another surgery which may only serve to make things worse.


Walking down the street and nothing happens!
Well this is what it was all about really, and in many ways, I wasn’t really prepared for it! I had spent most of my life aware that I looked different, and I knew that people picked up on that (whether they chose to mention it or not was their prerogative) – I sensed it by the subtle stares that lasted a little bit too long, or the somewhat jarred quickly turning away to the much less subtle people pointing and laughing to their friends “Look Chloe, I can see your husband over there.” or to the straight out harassment “Hey, Pinocchio, I can see you’ve been telling a lot of lies.” (I used to love Pinocchio by the way, but nasty people have ruined it for me). After the rhinoplasty, and once I was well on the road to recovery and started resuming a lot of my normal duties, I started to sense a change in the air. I walked down the street and I didn’t get this sense that people were staring – people would look at me no differently to other people. It’s strange to describe how liberating it feels to not be noticed, to be able to just fit into a crowd and no-one thinks twice. Of course, emotionally, there’s a lot of scars that still need addressed, but feeling that I now have the control to decide when I address the fact that I was born with a cleft is empowering. Naturally, I have nothing to hide, and am very open with people I care about regarding the fact I was born with a cleft (it is nothing to be embarrassed about after all), but to not have to explain my life history to a girl I’ve just met in a kitchen at a campsite and instead talk confidently about my favourite hiking spots is a sign of a good rhinoplasty outcome.

Discover more from Kenny Ardouin
Subscribe to get the latest posts sent to your email.

Interesting read. I am a sixty-three year old male born with a unilateral left Cleft Lip and Palate. I had the septoplasty and it helped greatly, re: the problems you alluded to. The one unexpected thing was, by opening up those passages, it was like the monkey house at the zoo. It took weeks for the stink to dissipate. I have a small fistula and a rib graft was tried and failed. Now use a water pik.
LikeLike